Before you continue reading this blog, take a moment and reflect for one moment: what do you, as a clinical psychologist, use as a criterion for recovery or therapy success? Do you mainly focus on recovery from symptoms? Or do you use broader criteria, like whether the client is feeling well, and able to develop as a person and be part of community? Scientific studies into mental health have had a major focus on the first, more clinical aspects of recovery, while the second, broader perspective, recovery in terms of mental wellbeing, has gained much less attention. However, the concepts of recovery and mental health have been changing over time (Bohlmeijer & Westerhof, 2021). This blog reflects on this topic and the use of a validated measurement instrument to help you measure mental wellbeing (Iasiello et al., 2022).
What would it mean for clinical psychology if we maintained an intentional focus on both treating mental illness and promoting mental wellbeing? While early clinical psychology had a clear focus on positive functioning, the field has become primarily focused on the assessment and management of dysfunction and distress (Joseph & Wood, 2010; Keyes, 2005). Think of Roger’s fully functioning or Maslow’s self-actualization; these are some of the concepts that lay the foundation for modern psychology and the research supporting a focus on what makes life worth living.
The past two decades have seen a rise in attention on mental wellbeing in the literature, which has reoriented psychology back toward positive functioning in addition to a focus on distress and impairment (Keyes, 2005). Mental wellbeing is becoming integrated into clinical practice to achieve sustainable mental health (Bohlmeijer & Westerhof, 2021), with development of wellbeing oriented therapies (e.g., wellbeing therapy by Fava & Ruini, 2003) to transform a deficit-focused approach towards a more strength- and human-potential based one (Maddux, Snyder, & Lopez, 2004).
While the integration of wellbeing into clinical psychology has come a long way, more work is needed before this approach will be widely adopted and even including into clinical training programs. The inclusion of therapeutic techniques and practice to build wellbeing should also be extended to assessment of mental wellbeing in clinical populations. Joseph and Wood (2010) outlined three potential reasons to assess mental wellbeing in clinical practice:
- To assess whether current clinical practice is already engaged in improving mental wellbeing,
- To develop new approaches and techniques designed to improve mental wellbeing, and
- To increase the ability to treat distress and dysfunction.
Evidence now supports these three rationales, as studies have shown that both traditional clinical approaches (e.g., Cognitive Behavioral Therapy, CBT) and novel wellbeing-specific interventions (e.g., mindfulness and positive-psychology interventions) can improve mental wellbeing in clinical populations (van Agteren et al., 2021). Further, mental wellbeing may introduce new therapeutic targets for clinicians, particularly for clients with recurrent or chronic mental illness and where clinical recovery is unlikely. We argue that there is a sufficient body of evidence to warrant the complementary assessment of mental wellbeing in clinical practice (for those interested see Iasiello et al., 2020).
There are a multitude of assessment tools for wellbeing available, which for use in clinical practice (and the general population) needs to be well validated. To this end, we conducted a review of a well-validated and popular measure of mental wellbeing, the Mental Health Continuum – Short Form (MHC-SF; Keyes et al., 2008), to investigate whether the factor structure was consistent across clinical and non-clinical populations.
We chose the MHC-SF because, using only 14 questions, it can assess three theoretically derived aspects of mental wellbeing and be used to calculate a total wellbeing score (Keyes 2005). Other measures of wellbeing of a similar length are less grounded in clinical, humanistic, social and positive psychological theories and have only demonstrated a ‘general wellbeing score’, so we believe the MHC-SF has greater relevance in clinical practice. These three aspects of wellbeing are:
- Emotional wellbeing: referring to judgements of satisfaction with life, happiness, and interest in life
- Psychological wellbeing: referring to positive functioning of the individual, tapping concepts such as a sense of meaning and purpose, self-esteem, and warm relationships with others.
- Social wellbeing: referring to an individual’s judgement of their society around them, as well as their perceived contribution and connection with communities.
Using a novel assessment technique, called Meta-analytic Factor Structural Equation Modelling, we were able to extract the data from more than 100,000 participants in over 26 studies from around the world to evaluate the factor structure of the MHC-SF (Iasiello et al. 2022). We showed that the hierarchical model (Figure 1) was supported statistically and theoretically and performed similarly across clinical and non-clinical cohorts. One caveat of our analysis was that there were differences in the loading of items on each of the three aspects of wellbeing between clinical and non-clinical groups, therefore caution is required when comparing scores between groups.
To better understand how a wellbeing measurement can be used to enhance clinical practice, consider two clinical case examples. For example, consider Mrs. Jones, who is in therapy for generalized anxiety disorder. The outcome measurement shows that she recovered well in terms of a reduction in anxiety symptoms. However, the scores on the MHC-SF show that she improved somewhat on mental wellbeing, but still scores below average, in particular on psychological wellbeing. In this case, would it make sense to offer an intervention aimed to promote her mental wellbeing, like well-being therapy that specifically targets psychological wellbeing (Fava & Ruini, 2003). This might not only support Mrs. Jones in preventing relapse of the anxiety disorder, but also to live a life worth living.
Alternatively, consider Mr. Frank, who is in treatment for a long-term personality disorder. His scores on the MHC-SF are really low. As a clinician you might judge this might interfere with a good therapy outcome in terms of symptom reduction. In this case, could you consider complementing therapy with activities that boost wellbeing, for instance by focusing on building meaning or working on their social wellbeing? This might give Mr. Frank further resources in dealing with his disorder and contribute to a better progress in therapy.
It’s been said a million times, mental health is more than the absence of mental illness. If clinical psychology wants to return to a focus on the promotion of mental wellbeing and positive functioning, it is vital that it also includes mental wellbeing in its assessment. This is because it’s insufficient to attempt to infer mental wellbeing from the absence of mental illness (Franken et al. 2018). Our study has demonstrated that it’s appropriate to use the MHC-SF in clinical populations, and that it can be used to tap into three clinically relevant aspects of mental wellbeing. Therefore, we hope that this review, and related literature, builds clinician confidence to include measures of mental wellbeing in the overall assessment their clients.
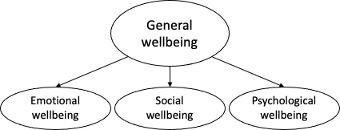
Figure 1: Hierarchical model of the Mental Health Continuum – Short Form
Target Article
Iasiello, M., van Agteren, J., Schotanus-Dijkstra, M., Lo, L., Fassnacht, D. B., & Westerhof, G. J. (2022). Assessing mental wellbeing using the Mental Health Continuum—Short Form: A systematic review and meta-analytic structural equation modelling. Clinical Psychology: Science and Practice. Advance online publication. https://doi.org/10.1037/cps0000074
Discussion Questions
- Which aspect of mental wellbeing is most relevant to your clinical specialty?
- Would your clients benefit from a focus on improving wellbeing as a complement to mitigating and treating distress and dysfunction?
- Are you ready to begin assessing wellbeing in your clinical practice? If not, what further evidence would you need to see?
About the Authors
Matthew Iasiello is a mental health and wellbeing researcher, based at the South Australian Health and Medical Research Institute (SAHMRI). Matthew is a senior researcher the Be Well Co, a start-up initiative focused on dissemination of preventative and early intervention mental wellbeing interventions in the community. He is currently in the process of submitting his PhD Thesis at Flinders University, focused on the relationship between mental wellbeing and mental illness.
Professor Gerben Westerhof is chair of the group Psychology, Health, and Technology and director of the Story Lab at the University of Twente, the Netherlands. He is mainly interested in how personal storytelling contributes to lifespan development, mental health and well-being. He was involved in the development and evaluation of several narrative interventions, like life review therapy. He has been involved in studies on the Mental Health Continuum – Short Form and its implementation in mental health care. [I’ve just added the names of those who replied with interest in the blog]
Dr Daniel Fassnacht is a Lecturer in Psychology at the College of Education, Psychology and Social Work, Flinders University, Adelaide. He further holds an Honorary Research Fellow at The Australian National University, Canberra, and an Associate Research Fellow at the South Australian Health and Medical Research Institute. Dr. Fassnacht has extensive academic experience having held five teaching and research appointments internationally over a twelve-year period. Dr. Fassnacht has significant expertise and experience in developing digital tools to address mental illness and promote wellbeing including Internet-based prevention and intervention programs
Joep van Agteren is the co-lead for the Mental Health and Wellbeing program at the South Australian Health and Medical Research Institute (SAHMRI) and an affiliate research at the Órama Institute for Mental Health and Wellbeing. His work centres around the use of evidence synthesis to research innovations in the way we conduct mental health interventions and measurement. His work has a strong applied focus, by developing new solutions that are being disseminated into the community via a start-up called Be Well Co.
References Cited
Bohlmeijer, E.T., & Westerhof, G.J. (2021). The model for sustainable mental health: Future directions for integrating positive psychology into mental health care. Frontiers in Psychology, 12. https://doi.org/10.3389/fpsyg.2021.747999
Fava, G. A., & Ruini, C. (2003). Development and characteristics of a well-being enhancing psychotherapeutic strategy: Well-being therapy. Journal of Behavior Therapy and Experimental Psychiatry, 34(1), 45-63. https://doi.org/10.1016/s0005-7916(03)00019-3
Franken, K., Lamers, S. M., Ten Klooster, P. M., Bohlmeijer, E. T., & Westerhof, G. J. (2018). Validation of the Mental Health Continuum‐Short Form and the dual continua model of well‐being and psychopathology in an adult mental health setting. Journal of clinical psychology, 74(12), 2187-2202.
Iasiello, M., van Agteren, J., Muir-Cochrane, E. (2020). Mental health and/or mental illness: A scoping review of the evidence and implications of the dual-continua model of mental health. Evidence Base (1), 1-45.
Joseph, S., & Wood, A. (2010). Assessment of positive functioning in clinical psychology: Theoretical and practical issues. Clinical Psychology Review, 30(7), 830-838. https://doi.org/10.1016/j.cpr.2010.01.002
Keyes, C.L., 2005. Mental illness and/or mental health? Investigating axioms of the complete state model of health. Journal of Consulting and Clinical Psychology, 73(3), 539–548. https:// doi.org/10.1037/0022-006X.73.3.539.
Keyes, C.L., Wissing, M., Potgieter, J.P., Temane, M., Kruger, A., van Rooy, S., 2008. Evaluation of the mental health continuum-short form (MHC-SF) in Setswana-speaking South Africans. Clinical Psychology and Psychotherapy, 15 (3), 181–192. https://doi. org/10.1002/cpp.572
Maddux, J. E., Snyder, C. R., & Lopez, S. J. (2004). Toward a Positive Clinical Psychology: Deconstructing the Illness Ideology and Constructing an Ideology of Human Strengths and Potential. In P.A. Linley and S. Joseph (Eds.), Positive Psychology in Practice, John Wiley & Sons. https://doi.org/10.1002/9780470939338.ch20.
van Agteren, J., Iasiello, M., Lo, L., Bartholomaeus, J., Kopsaftis, Z., Carey, M., & Kyrios, M. (2021). A systematic review and meta-analysis of psychological interventions to improve mental wellbeing. Nature Human Behaviour, 1-22. https://doi.org/10.1038/s41562-021-01093-w
Interested in submitting a blog post?
Link HERE to download the SCP Blog Submission Form
