Adolescence is an important developmental period during which youth experience key changes in their ability to regulate emotions and behavior, and engage in more reward-seeking and risk-taking behaviors than during childhood (Andrews et al., 2021; Steinberg et al., 2008). Adolescents who have difficulties with emotional and behavioral regulation are at elevated risk for externalizing problems (e.g., defiance, aggression, impulsivity, antisocial behaviors).
Although externalizing problems are a common reason for psychiatric referrals (Connor et al., 2019), only a minority of youth with these difficulties receive interventions with strong research support (McCart & Sheidow, 2016). We evaluated evidence as to whether interventions based on Dialectical Behavior Therapy (DBT), a well-studied intervention designed to reduce destructive behavior by enhancing ability to regulate emotions, may reduce externalizing symptoms among adolescents. Despite DBT’s focus on changing thoughts and behaviors that precede and relate to interpersonal conflict, externalizing problems are rarely examined as a primary aim in DBT-based intervention studies.
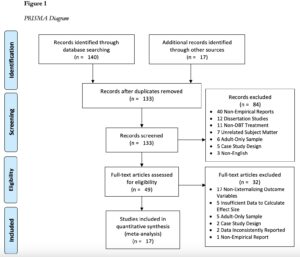
Systematic searches of peer-reviewed articles were performed on two electronic databases through February 2022. See Figure 1 for a diagram depicting the search strategy and selection procedures (click to enlarge):
Seventeen studies reporting on 16 independent samples across 5 countries were included. Each study collected data on at least one relevant outcome variable, resulting in 25 data points. In terms of covariates, we examined setting, country, study design, average age of participating adolescents, duration of intervention, number of skills group sessions, number of overall sessions, availability of phone/milieu coaching, inclusion of family members in DBT skills groups, presence of intervention modification, and reporter for the outcome variable.
Results suggested that DBT-based interventions hold promise for reducing externalizing symptoms among adolescents (Hedge’s g = -.499; see Figure 2 for forest plot [click to enlarge]), and that variability in outcomes may be explained by features of the studies.
Additionally, intervention duration (but not number of skills groups or overall sessions) moderated the overall effect, suggesting that a longer period of participation in treatment has a beneficial impact on adolescent externalizing symptoms regardless of the total number of skills groups or overall sessions. However, the moderating role of intervention duration approached but was no longer significant (p = .057) following removal of an outlier. No other hypothesized moderators impacted the overall effect of DBT-based interventions on externalizing symptoms.
We hope that future DBT research will continue to investigate externalizing symptom outcomes among adolescents with thoughtful inclusion of potential moderators, as well as evaluate adolescents who meet criteria for disruptive behavior disorders given DBT’s potential effectiveness for youth who might not currently receive DBT.
Target Article
Jakubovic, R. J., & Drabick, D. A. G. (2023). Dialectical behavior therapy-based interventions for externalizing problems among adolescents: A meta-analysis. Clinical Psychology: Science and Practice. Advance online publication. https://doi.org/10.1037/cps0000140
Discussion Questions
- If you were to design a study of a DBT-based intervention for adolescents with externalizing problems, what potential predictors of better treatment outcomes would be important to study?
- If you were to conduct a dismantling study where only some modules were applied to adolescents, which DBT skills or components of DBT do you hypothesize would be most beneficial for adolescents with externalizing problems?
- What are some potential barriers to implementing DBT-based interventions (or assessing the effectiveness of those interventions) with adolescents across settings (e.g., inpatient, community, correctional, educational settings)?
- Given elevated levels of co-occurring symptoms among adolescents with externalizing problems (e.g., depressive symptoms, substance use), how might co-occurring symptoms be incorporated into intervention efforts?
About the Authors
 Rafaella J. Jakubovic, M.A. is a doctoral candidate in the Clinical Psychology Ph.D. program at Temple University. Rafaella earned her Bachelor’s degree in Psychology at the Tulane University Honors Program in 2016 before matriculating at Temple, where she completed her Master’s degree in 2018. She can be reached by email at rjakubovic@temple.edu and on Twitter @Rafi_Jakubovic.
Rafaella J. Jakubovic, M.A. is a doctoral candidate in the Clinical Psychology Ph.D. program at Temple University. Rafaella earned her Bachelor’s degree in Psychology at the Tulane University Honors Program in 2016 before matriculating at Temple, where she completed her Master’s degree in 2018. She can be reached by email at rjakubovic@temple.edu and on Twitter @Rafi_Jakubovic.
 Deborah A. G. Drabick, Ph.D. is an Associate Professor in the Department of Psychology and Neuroscience at Temple University. She also leads the Child Health and Behavior Lab and her research uses a developmental psychopathology perspective to examine risk and resilience, contextual processes, typical and atypical development, developmental trajectories, co-occurring conditions, and preventive interventions across the lifespan. Further information can be found here: https://sites.temple.edu/drabicklab/projects/ and Dr. Drabick can be reached at ddrabick@temple.edu.
Deborah A. G. Drabick, Ph.D. is an Associate Professor in the Department of Psychology and Neuroscience at Temple University. She also leads the Child Health and Behavior Lab and her research uses a developmental psychopathology perspective to examine risk and resilience, contextual processes, typical and atypical development, developmental trajectories, co-occurring conditions, and preventive interventions across the lifespan. Further information can be found here: https://sites.temple.edu/drabicklab/projects/ and Dr. Drabick can be reached at ddrabick@temple.edu.
References
Andrews, J. L., Ahmed, S. P., & Blakemore, S. J. (2021). Navigating the social environment in adolescence: The role of social brain development. Biological Psychiatry, 89(2), 109-118. https://doi.org/10.1016/j.biopsych.2020.09.012
Connor, D. F., Newcorn, J. H., Saylor, K. E., Amann, B. H., Scahill, L., Robb, A. S., Jensen, P. S., Vitiello, B., Findling, R. L., & Buitelaar, J. K. (2019). Maladaptive aggression: With a focus on impulsive aggression in children and adolescents. Journal of Child and Adolescent Psychopharmacology, 29(8), 576–591. https://doi.org/10.1089/cap.2019.0039
McCart, M. R., & Sheidow, A. J. (2016). Evidence-based psychosocial treatments for adolescents with disruptive behavior. Journal of Clinical Child & Adolescent Psychology, 45(5), 529–563. https://doi.org/10.1080/15374416.2016.1146990
Steinberg, L. (2008). A social neuroscience perspective on adolescent risk-taking. Developmental Review, 28(1), 78–106. https://doi.org/10.1016/j.dr.2007.08.002